|
What does it feel like?
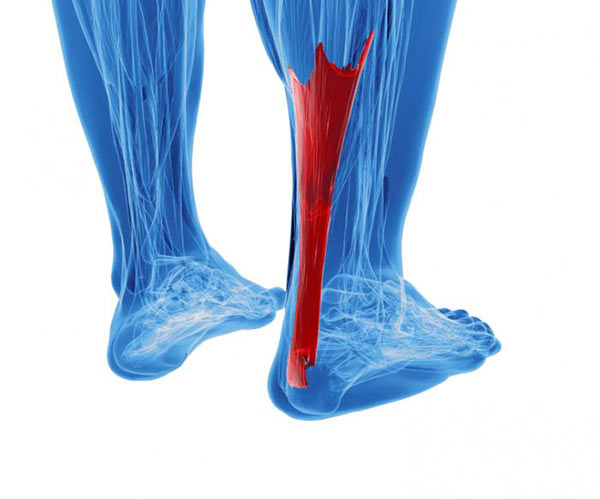
Achilles tendinopathy presents as a aching pain or tightness across the back of the heel, It usually feels at its worst of a morning or after a prolonged period of rest. Sometimes after a warm up the tendon can actually feel better, but will then ache again after a cool down or the day after exercise. How does it work? The achilles tendon is the strong connective tissue that connects the calf muscle to the back of the heel. This allows for pushing the toes into the floor and adsorbing ground reaction forces when walking or running. It is made up of strong fibers called collagen. Those fibers are broken down when high forces are placed on the tendon (exercise). In response to this, with enough rest time, the body lays more collagen down to replace it, plus usually a little more to prepare the body for future bouts of exercise. If this cycle is repeated the tendon can continue to get stronger and stronger. However, when the amount of time between each bout of exercise isn’t enough, or the exercise is too much, the body will not be able to keep up, and the tendon is gradually broken down. What can be done? Below are a few tips on what will help/ harm an achilles tendon. A proper assessment from a physio will also help unravel some of the underlying reasons this may have arisen in the first place. A physio will also be able to guide you on the correct type and amount of exercise to perform to get better. Things tendons like:
If you or someone you know may need a physio on the central coast to treat this condition then please do get in touch.
1 Comment
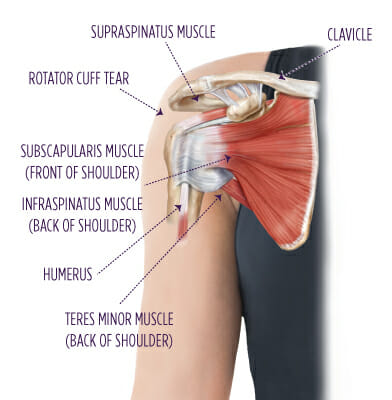
First of all, what is a rotator cuff?
Rotator cuff muscles are 4 small muscles that help to hold the arm in the in the shoulder socket while bigger muscles perform movement. The shoulder is a ball in socket joint which means it is highly mobile but somewhat instable. That is why these muscles are required to add additional stability. How do they tear? Rotator cuff tears usually come about when the shoulder sustains a sudden stretch or is over exerted such as a heavy lift or throwing manoeuvre. Does a tear repair? Usually not, that’s why sometimes tears in the rotator cuff can appear on ultrasound or MRI imaging even years after they were sustained. That’s ok though, usually the tear only makes up part of the muscle, so the rest of the muscle and the other surrounding muscles can compensate. Most of the time people with a rotator cuff tear wont even know its there. In one study of baseballers, 83% of players with a tear in one or more rotator cuff muscles on ultrasound did not have any symptoms or pain. What do I do if I have a sore shoulder? As mentioned above, a rotator cuff tear may be present for years without much issue, the problem will come when you decide to try something strenuous with the shoulder that it isn’t used to. This usually comes at the start of a sports season, renovating a house or some other infrequent or once off bout of exercise. Given that rotator cuff tears are so common, even in people without pain. It won’t be all that helpful to get an image of the sore shoulder. In fact, physios can usually get all the necessary information needed from a physical assessment and a history of your pain or discomfort. If it doesn’t repair, then how do I fix my shoulder? If part of a rotator cuff is torn, then the job now is to strengthen the remaining fibres of that muscle, as well as the other muscles in the system. This is especially important when you have a painful shoulder, but as a preventative measure it is also a good idea to keep good strength in the system. Physio will be able to set and progress a good exercise program appropriate to you.
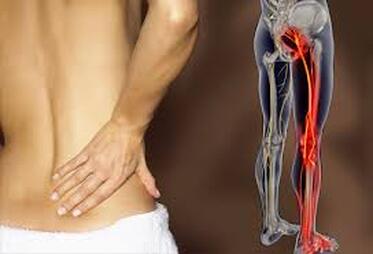
What does it feel like? Sciatica presents as a pain starting at the lower back or hip and can progress down the leg, in some cases all the way down to the feet. Sometimes there is associated numbness and/or pins and needles. This pain can feel like a deep ache that won’t go away and can become worse in certain positions, typically sitting and movements bending forward. Any symptoms such as numbness in the inner thigh or groin and/or change to bowel or bladder function are considered more serious and should be directed to medical attention. What is it? Sciatic pain comes about when there is pressure or tension on any of the nerves that run from the lower spine into the leg. Nerves in the lower body start at the spine (nerve roots) run down to a point around the buttock where they bunch together (sciatic nerve) then spread out around the lower limb. These nerves are responsible for sensation of pain, touch, temperature and movement. If a nerve is being put under pressure or irritated somewhere along this pathway it will result in pain and potentially disruption to the other signals (sensation and strength) Why does this happen. There are two main causes for sciatic pain. The first is when the nerve root is pressed on by a disc as it exits the spinal cord in the lower back. The second common cause is when the sciatic nerve bunch is pressured by the piriformis muscle around the hip/buttock area. A physio assessment will be able to determine which one of the above is the cause in each case. Depending on where your sciatic pain originates, the cause and treatment can go from there. Can it be fixed? Yes, it can! Physio treatment for sciatic pain usually aims to address the positions or movements that may contribute to nerves being pressured, and exercise to help mobilise the nerve so it can glide smoothly through its pathway. Usually some improvement can be seen right away but symptoms may linger for some time. If treated early symptoms usually resolve much quicker and more invasive treatment won’t be required. Lateral epicondylalgia (Tennis elbow) What does it look/ Feel like? Pain around the outside of the elbow / forearm. Usually worse first thing in the morning or at the beginning of tasks, then warms up as you get going. It can be quite a sharp pain when lifting or squeezing (something simple like lifting a shopping bag or coffee mug) but can ache after a solid bout of activity. What is it? Tennis elbow is aggravation of the extensor tendons of the wrist/ hand. The muscles that move the wrist and hand are long, they start around the elbow. Tendons can become aggravated when they are over worked, if they sustain a blow (bumping the elbow) or when they are placed on stretch. What causes it? As mentioned above, any activity that places sudden high loads on the wrist extensor tendons, stretches them or a bump to them. An obvious example is tennis, but even occupational activities such as lifting with overhand grip or handwriting can lead to a progressively worsening pain. Sometimes this process can be kickstarted by simply bumping the outside of the elbow then adding too much activity afterwards. Can it be fixed? Yes! It certainly can. The best researched treatment for tennis elbow includes a combination of progressive strength exercises, managing load (how much exercise /aggravating activity performed) and adapting the way you perform tasks around the house or work. Other therapies such as tape and bracing can also help begin the healing process. How long will it take? Usually if treated early, improvement can be noticed within the first few weeks and final symptoms resolve in around 6-8 weeks. This process can be a bit slower if the symptoms have been present for a while. Treatment can also be dragged out if reducing or adapting aggravating activities does not take place. What is it?
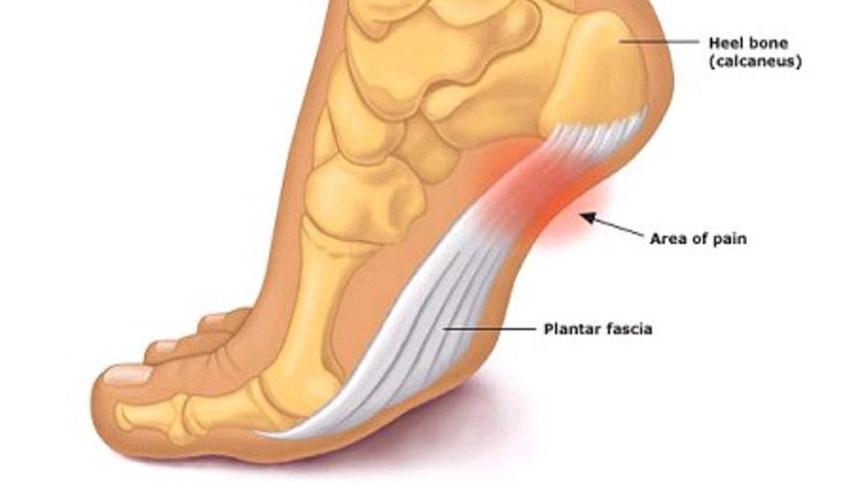
Plantar fasciitis is a condition affecting the long tendon like fascia that runs directly under the sole of the foot, running from the heel to the base of the toes. It is characterised by pain felt along the sole of the foot. This pain is typically worst of a morning and can feel better after a bit of a warm-up. What is the Cause? The Plantar fascia gets broken down when the stress on it is too great for the body to cope with. This may be due to an increase in total activity (like returning to pre-season training) or when it has to take more of the normal load than its used to (like a change in the way you walk/run or a new pair of shoes). As we get older our body has less ability to adapt to these subtle changes in load. Can it be fixed? How? Yes! The body has an amazing ability to adapt and change. The best course of action is to modify or manage how much activity you are doing, and gradually build up the tissue so it is strong enough to meet the demands you wish to place on it. How does that work? The plantar fascia is made up of strong fibres called collagen, which are damaged during exercise. in times of increasing demand on the plantar fascia the body lays down more of this collagen to make it stronger. When exercise load increases too suddenly, the body is unable to keep up, and instead of slowly building up, the collagen slowly gets broken down. Do I need to stop running/ Exercising? No! its important not to over do it, but it is also important to keep some exercise going, otherwise the plantar fascia won’t get stronger, it will get weaker. How can a Physio help? Physiotherapists will be able to guide you through a targeted exercise therapy program designed at building strength in the plantar facia. Your physio will also be able to guide and manage your exercise load through this period. In some cases, adapting the way you move will help reduce the amount of pressure you place on the plantar facia when walking or running. This may be done through biomechanical analysis or by adaptive measures such as taping or orthotics. How do I get in to see a physio?
Anyone is free to book in to see their local physio. You don’t need to be referred from your GP to begin with. In some cases, your local physiotherapist is the best place to start when it comes to a muscle or joint injury. What if I can’t afford physio? In some cases, your local GP can refer you to physiotherapy with an EPC (Enhanced Primary Care plan) This will entitle you to physiotherapy sessions payed for in part by medicare. Who is eligible for an EPC? An EPC is issued at a GPs digression to a person with a chronic condition (greater than 3 months) or a condition that may become chronic. The aim of an EPC is to treat a person’s injury with physio before it becomes a greater problem or limits their health. This could be a chronic lifestyle disease like diabetes, heart disease or Parkinson’s disease. Or it could be something like ongoing lower back pain or shoulder pain that is limiting from you keeping fit and healthy. How Can Physio Help me? Physiotherapists are musculoskeletal experts, which means they are your best port of call when it comes to anything to do with muscle, bone, nerve issues and joint pain, we also have a wealth of knowledge about chronic lifestyle conditions and exercise prescription. Physiotherapy usually involves hands on treatment like massage or dry needling and a strong focus on exercise therapy. What else can physios help with
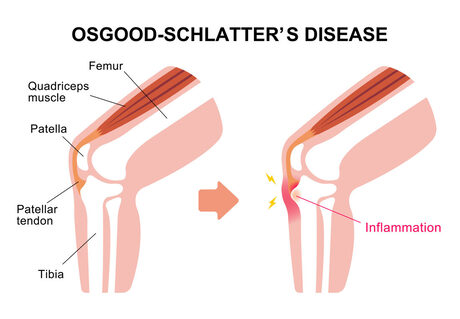
If this sounds like you, come in or give us a call to see how else physio on the central coast may help you. Osgood-Schlatters disease is one of a group of injuries known as a traction apophysitis. This is when a tendon pulls on the growth plate of the bone, pulling a small portion of it away. In the case of this condition it is the patella tendon pulling away from the front of the shin. Why does it happen. There is a range of reasons this can occur. As mentioned, one factor can be a phase of increased growth. When the body grows not all tissue grows at the same rate, meaning the muscles and tendons can take a little while to catch up to the growth of bones. Another factor is muscle and tendon loading, this generally means sport. There will be a direct relationship between the amount of sport performed week to week and the likelihood and amount of pain this issue can cause. What happens if I have Osgood-schlatters? Osgood-schlatters comes on usually in early to mid-teen years and hangs around for a 6-18 months before disappearing when growth slows down again. At times pain will be worse than others when sports load or growth is at its most. The main goal through those episodes is to manage how much sport is performed so the athlete can get out and do the most important things like weekend games. What can be done about it? The main goal of treatment is to give strength to the areas surrounding the knee, and to take load away from the patella tendon itself. Taking load away may include reducing the amount of sport, taping / braces or looking at movement mechanics to make sure force is being dispersed evenly across the knee. Can it be cured? Generally, the symptoms resolve after 6-18 months when bones begin to fuse and growth slows. In the mean-time it can be managed so it doesn’t get so bad you have to stop playing sport all together. Most of the time pain will limit any serious progression, in rare cases the bone can pull away completely. |
Archives
December 2021
Categories |
Proudly powered by Weebly



 RSS Feed
RSS Feed